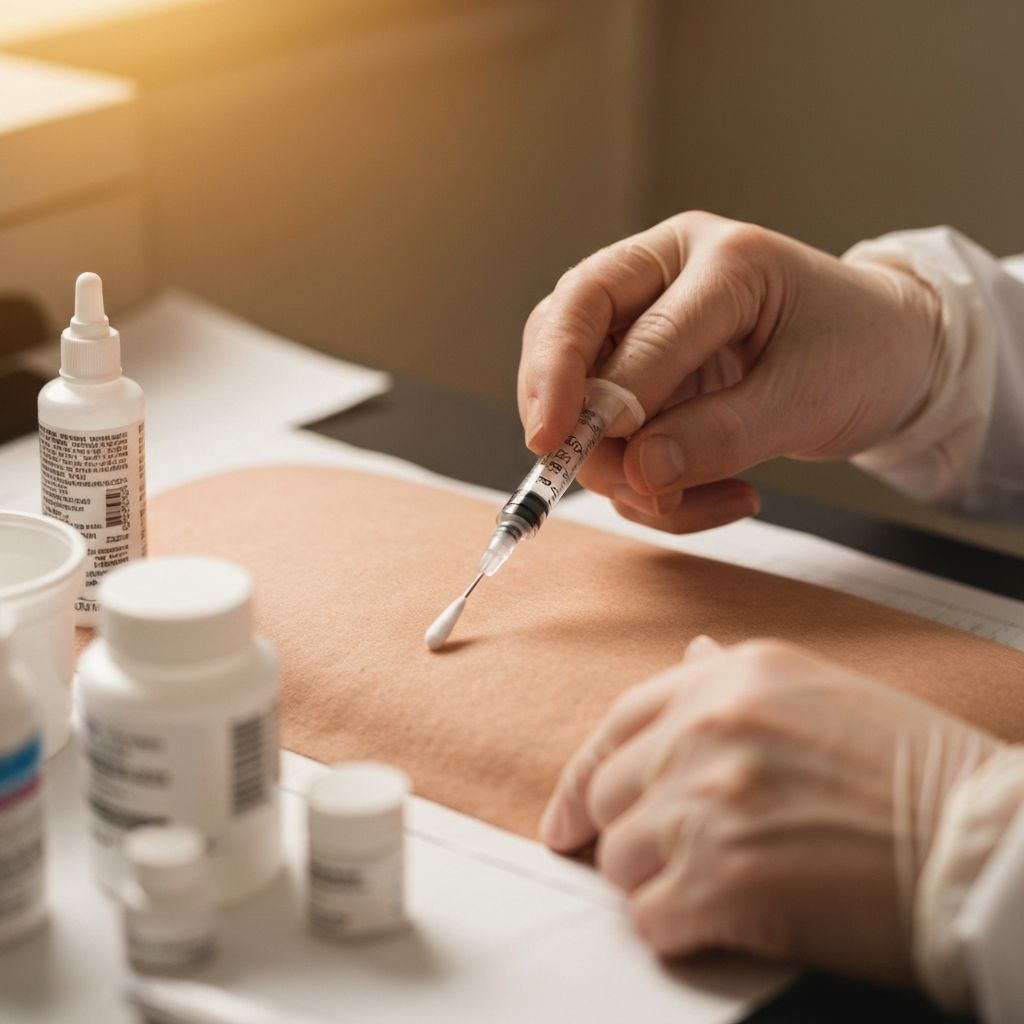
Subcutaneous vs. Intramuscular
Most peptides are administered subcutaneously (into the fat layer under the skin). This method is easier, less painful, and appropriate for the vast majority of peptides. Intramuscular injection is rarely needed for peptides.
DYK Data: 94% of community peptide injections are subcutaneous. IM injection is typically only used for specific growth hormone protocols.
| Method | Needle Length | Needle Gauge | Best For |
|---|---|---|---|
| Subcutaneous | 5/16" (8mm) | 29-31G | Most peptides (BPC-157, TB-500, GLP-1s) |
| Intramuscular | 1-1.5" | 23-25G | Some GH protocols (rare for peptides) |
Subcutaneous Injection Guide
- Step 1: Wash your hands thoroughly with soap and water
- Step 2: Clean the injection site with an alcohol swab and let it air dry
- Step 3: Draw your dose into an insulin syringe, removing any air bubbles
- Step 4: Pinch a fold of skin between your thumb and forefinger
- Step 5: Insert the needle at a 45-90° angle (90° for short insulin needles)
- Step 6: Slowly depress the plunger over 5-10 seconds
- Step 7: Release the skin fold, then withdraw the needle
- Step 8: Apply light pressure with a clean cotton ball if needed
Injection Site Rotation
Rotate injection sites to prevent tissue damage and ensure consistent absorption. Common subcutaneous sites include:
- Abdomen (most common) — avoid 2 inches around the navel
- Outer thigh — front/outer area, middle third
- Back of upper arm — pinch required or use helper
- For localized healing peptides (BPC-157): inject near the injury site
Safety Tips
- Never reuse needles — use a fresh needle for each injection
- Always use alcohol swabs on both the vial and injection site
- Store needles in a sharps container and dispose properly
- If you see blood when drawing back, you've hit a vessel — withdraw and retry
- Slight burning or stinging is normal for some peptides